 |
 |
1. Why Should I Do A Self-Exam?
There is a greater than 1 in 10 chance that a woman will contract breast cancer at some point over her lifetime, and over 1,000,000 women find lumps in their breasts (some cancerous, most benign) every year. While these statistics are alarming, a simple Breast Self-Examination (BSE) could be the key to finding any abnormality early on. And since the American Cancer Society and the Breast Cancer Fund still recommends that women aged 20 and older should conduct Breast Self-Exam on a monthly basis, it is never too soon to learn how to do it right.
The purpose of a Breast Self-Exam is for you to learn the topography of your breasts. Knowing how your breasts normally feel will allow you to notice changes in the future.
If found early enough, almost 95% of all cases of breast cancer can be effectively treated. That's why the BSE is so important.
ANYTHING you can do to help you find something early will greatly increase your chances of getting effective and proper treatment for the cancer.
Remember: The BSE should be used in combination with mammography (an X-ray of your breast) and the Clinical Breast Examination (CBE -when an experienced doctor examines your breasts). Women should never use BSEs as a substitute for mammography or CBEs, because while it's really easy to do a BSE, it's also the least precise method.
Risk Factors
You can't get breast cancer from bumping or bruising your breast, nor can you catch breast cancer from someone else, like the chicken pox. Rather, there are several risk factors which will determine how likely you are to contract breast cancer. Below, we talk about the main ones, in order of their importance: age, family history, personal history, and lifestyle.
Age
Breast Cancer is rarer for women younger than 35 (the risk for the disease increases exponentially by age). Most breast cancers occur in women older 50. The risk of developing breast cancer in the next year
- Age /Risk
- 20-24 /1 in 110,000
- 25-29 /1 in 12,850
- 30-34 /1 in 3,700
- 35-39 /1 in 1,555
- 40-44 /1 in 790
- 45-49 /1 in 531
- 50-54 /1 in 450
- 55-59 /1 in 386
- 60-64 /1 in 292
- 65-69 /1 in 244
- 70-74 /1 in 215
- 75-79 /1 in 215
- Source: National Cancer Institute
Family History
If your mother, sister, or daughter has developed breast cancer before menopause, you are three times more likely to develop the disease. If two or more close relatives (e.g., cousins, aunts, grandmothers) have/had breast cancer, you are at increased risk as well. Recently, scientists have found that mutations in genes BRCA1 and BRCA2 increase one's susceptibility to breast cancer. A simple blood test can tell you if you have such a condition.
Personal History
If you've had breast cancer, you have an increased risk of getting it again. Also, if you've had benign breast disease (e.g., fibrocystic breast disease), you are at an increased risk. The following also put you at greater risk:
- If you began menstruating early (before age 12)
- If you take birth control pills (though evidence is not conclusive)
- If you never have children
- If you have children when you are 30 or older
- If you have menopause at 55 or older
- If you take Hormone Replacement Therapy (HRT)
As you may have noticed, most of these risk factors involve your level of estrogen. Higher estrogen levels are strongly linked with susceptibility to breast cancer.
Lifestyle
There have been several studies that found a lower incidence of breast cancer among women who exercise regularly and a higher proportion of breast cancer among obese women. There is also evidence that there is increased risk of breast cancer with increased alcohol use (i.e., 3 or more drinks per week); perhaps due to the fact that alcohol increases blood estrogen levels.
Illustrations proivided by Julie Yu Chin Liu and are © 2000, SE Material/SoYouWanna.com, Inc.
2. How To Perform The Examination
You should conduct it once a month at about the same time each month. If you are a menstruating woman with regular cycles, it's best to conduct the BSE the week (2-5 days) after your period ends, because that's the point in your cycle when your breasts will be the least tender. If you have an irregular menstrual cycle, are pregnant, or have gone through "the change," you should pick the same date each month for your BSE (maybe the same day you pay your bills, so you'll remember).
There are two basic steps to conducting a BSE: first you look at your breasts (Visual Examination), and then you touch them (Tactile Examination).
Visual Examination
During the first part of the BSE, the visual examination, you are looking for changes in each breast. So if your breasts have always been mushy, that's not a concern unless this is a new change. The changes you are looking for include:
- Shape
- Size
- Contour or symmetry (is there a difference in the level between your nipples? Do both breasts look symmetrical?)
- Skin discoloration or dimpling
- Bumps/lumps - NOTE: normal lumpiness, like in the week before and of your menstrual cycle, will appear as very small and separate lumps like the texture of an orange.
- Sores or scaly skin
- Discharge or puckering of the nipple
Stand in front of a mirror and look for the above changes in your breasts (from both a frontal and profile view) in 3 different positions:
- With your arms up behind your head
- With your arms down at your sides
- Bending forward
- with your hands on your hips and shoulders turned in
- with your arms relaxed hanging in front of you
Tactile Examination
Don't be shy, this is the part of the examination when you need to feel your breasts for any changes. Regardless of your breast size, the examination is the same. The only exception is that large breasted-women should be sure they see and feel the entire breast and surrounding region, while very thin women should figure out whether the hard lump they've been feeling is just a rib bone or something of concern.
Begin by looking for the changes listed above while standing up. Some women find it useful to do this part of the BSE in the shower, since soap or bath gel will aid in the ease of feeling your breasts.
The first thing you have to do is pick a specific pattern. For the BSE, you need to pick a pattern to feel your breasts and surrounding areas, which include:
- the breast itself
- between the breast and underarm
- the underarm itself
- the area above the breast up to the collarbone and across to your shoulder
It is important to check surrounding areas because breast cancer may be found in the lymph node tissue around your breast and underarm.
You use the pads (where your fingerprints are) of your three middle fingers on your right hand pressed together flat to check your left breast, and do the opposite for the right breast. You should press on your breast with varying degrees of pressure:
- light (move the skin without moving the tissue underneath)
- medium (midway into the tissue)
- hard (down to the ribs "on the verge of pain")
When using any of the 3 patterns, you should always be using a circular rubbing motion (in dime-sized circles) without lifting up your fingers.
Patterns:
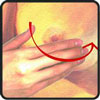
Spiral (concentric circles): begin with a large circle around the perimeter of your breast and make smaller and smaller circles as you work your way toward the nipple.
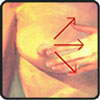
Pie shape wedges: pretend your breast is divided into sections like pieces of a pie, begin in the nipple area and feel your breast in a small circular motion within one pie shape section, then move on to the next wedge starting in the nipple area again.
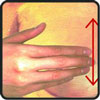
Up and down: pretend your breast is divided into vertical stripes, begin on one side and feel your breast in a small circular motion up and down in a zig zag pattern.
Then repeat the process for the other breast.
Once you've performed the tactile examination while standing up in front of a mirror, you should do the whole examination again, this time while lying down. Here's how to do so:
- Put your left arm behind your head and use your right hand to examine your left breast.
- Put a small pillow or towel under your left shoulder to aid you.
- Again, use the pads of your 3 fingers of your right hand to check your left breast in the pattern of your choice (spiral, pie shape wedges, or up and down).
- Be sure to always use the same pattern (it's the best way to know if there are changes).
- And again, don't forget to feel your breast using light, medium, and hard pressure.
- After you're finished, you must repeat the procedure again for your right breast.
3. What You Are Looking For
The purpose of this Self-Exam is to educate you about the topography of your breasts. Remember, you are looking for changes, so you need to collect a month or two of data before you really understand what change looks or feels like.
Here's what you might find:
Tender, lumpy breasts
This is usually part of your regular menstrual cycle due to swelling because you retain more water.
Overall small lumps and a bumpy/grainy texture
If this texture is found on both breasts in the area around your nipples and the upper and outer parts of your breasts, you may have fibrocystic breasts.
Single lump that feels like an oval and is hard on the outside, squishy on the inside
This may be a cyst. You can usually move a cyst under the skin and they sometimes produce a dull pain. A cyst is a fluid-filled sac that can vary in size from a pea to a half-dollar. Cysts appear most often in women aged 35 to 50 and increase as menopause approaches. They are benign.
Single, solid lump that feels round like a small rubber ball and can be moved
This may be a fibrodenoma, a benign and painless tumor made up of connective tissue and other cells. A fibrodenoma may vary in size from a marble to a lemon. They are more common in women in their late teens and early 20s or older women on Hormone Replacement Therapy.
Overall distinct large lumps
These may be just exaggerated lumpiness, called pseudolumps. These may be caused by scar tissue, a clump of fat cells, or an abscess (pus-filled sac). Sometimes nursing women experience mastitis, when bacteria enters the breast from dry cracks in the skin.
Single, solid lump that can NOT be moved
Look for hard, irregular borders to the lump. Also, determine if the lump appears in only one breast and if it remains the same size throughout your menstrual cycle. Note that thickened or dimpled skin is a sign of a lump that can NOT be moved (other benign lumps are movable because they are filled with fluid or lumps of fat). If all of the above occur, these are symptoms of breast cancer. Get it checked out immediately.
Sores or scaly skin
An open, itchy sore could just be a simple skin irritation (like from a new lacy bra that's cutting into you, or from switching your laundry detergent). However, in a few women, this could be a sign of Paget's disease, a rare form of breast cancer.
Discharge or puckering of the nipple
Persistent clear or bloody discharge from one nipple may indicate cancer in your breast ducts. Also, an inverted or puckered nipple (e.g., pulled back into the breast) may be a symptom of breast cancer.
4. Act If You Find Something
If you find that you exhibit any of the characteristics in step 3 (aside from normal menstrual lumpiness or retention of water), do not ignore your findings. Go see your physician immediately for a clinical breast exam and other tests. While some of the abnormalities we mentioned are usually benign, nothing is 100% and it's good to keep your doctor in the loop. Remember, the idea is to create a benchmarch and trackable history of the health of your breasts.
The first step your doctor will take will probably be a diagnostic test to exclude the possibility of cancer (either an ultrasound or a mammogram). An ultrasound uses high frequency sound waves to determine whether a lump is solid or fluid-filled. During a mammography, your breast is basically smooshed between 2 plates, which causes temporary discomfort, as an X-ray of your breast is taken.
After the ultrasound and mammogram, your doctor might rule out further testing and treatment. However, make sure you keep track of the changes you detected and that you have your doctor monitor these changes as well. More often, your doctor will want to get more information about your condition, like from a tissue or fluid sample. At this point, you may be referred to a specialist experienced in breast disease.
The following options are typical next steps :
Fine-needle aspiration
This is the least expensive and quickest test. It can be done in your surgeon's office with a local anesthetic. A needle syringe is inserted into the lump for a fluid sample. If clear fluid can be aspirated, that means it's a cyst. The aspiration procedure itself usually causes the cyst to disappear.
Needle biopsy
For this procedure, a needle syringe is inserted into the lump for a tissue sample. The sample is then sent to a lab where a pathologist determines whether cancerous cells are present.
Surgical biopsy
This procedure is what it sounds like. A surgeon operates to cut a small tissue sample of the lump. Then the sample is sent to lab pathologist to ascertain its status.
The next leg of the journey depends on your results from the tests above. Please make sure you feel comfortable with and confident in your doctor's abilities (and if you have any concern, get a second opinion). We wish you the best of luck and hope that this information has empowered you to feel more in tune with your body. Spread the word and tell your friends that a simple look & touch Breast Self-Exam just may save their lives.
Resources:
Breast Cancer Fund
1388 Sutter Street, Suite 400
San Francisco, CA 94109-5400
http://www.breastcancerfund.org
American Cancer Society
1-800-ACS-2345
http://www.cancer.org
National Cancer Institute
1-800-4-CANCER
http://www.nci.nih.gov




